
Introducing: Tip of the Month
Introducing our newest initiative – the ‘Tip of the Month’ feature on the Northwest Region Prehospital Care Program’s Learning Management System. Activate the QR code below for monthly insights, valuable tips, and expert guidance to enhance your prehospital care skills. Elevate your learning experience with our curated tips designed to empower and inform. Let the journey to continuous improvement begin!
Tip of the month
May 2026 - Tip of the Month - Amputations
Amputations are high-acuity, time-sensitive injuries that can occur in a wide range of environments; from industrial and farm machinery to motor vehicle collisions, power tools, and even sharp-force trauma. The mechanism can vary significantly, from clean surgical-like separations to severe crush or avulsion injuries, each presenting unique challenges for prehospital care. Regardless of the cause, early recognition and proper management are critical to patient outcomes. Effective hemorrhage control, preservation of the amputated part, when possible, and rapid transport decisions all play a vital role in improving survival and the potential for reattachment.
This month’s Tip of the Month is intended to support paramedics in assessing and prioritizing management of traumatic amputations, including effective hemorrhage control and appropriate preservation of the amputated part, in accordance with Ontario BLS and ALS-PCS standards.
You and your partner have been dispatched to a 38 year old male involved in a workplace accident. On arrival, you find the patient with complete amputation of three fingers on the left hand at the proximal phalanx, accompanied by significant hemorrhage. The patient appears pale, anxious, and in distress.
A coworker has retrieved the amputated digits and placed all three in a single bag directly on ice, which is handed to you on scene.
Questions we need to ask ourselves:
1) What are your immediate management priorities for this patient?
2) Is hemorrhage control adequate? If not, what additional interventions are required?
3) Has the amputated tissue been packaged properly? If not, what modifications are needed?
4) What elements are critical to include in your documentation?
Management Priorities:
“LIFE, LIMB, FUNCTION” Control hemorrhage, preserve tissue, minimize scene time where possible.
STOP THE BLEED
Pressure - pressure dressings- quick clot- tourniquet (if warranted)
- Re assess effectiveness of your care early and often, hemorrhage control is paramount.
MANAGE THE STUMP
With a COMPLETE amputation we need to cover the stump(s) in moist, sterile dressing and support with dry dressings on top. Immobilizing along with elevating can help manage this pt where it is possible.
With a PARTIAL amputation, we want to place in anatomical position(where possible) , and splint to prevent movement of body part. We need to be sure to assess and document the state of CSM distal to the injury/injuries.
PRESERVE THE PART - Critical Aspect
Rinse amputation of any gross contamination using sterile water, wrap the amputation in a moist, sterile dressing and place in a water tight, individual bag. We then need to place the amputation in an ice water slurry.
What we DO NOT WANT TO DO.
We want to avoid placing the amputated part directly on ice , we DO NOT want to soak the amputated part in water directly, and we DO NOT want to freeze this body part, just keep it cool.
Expected Actions
- Immediate hemorrhage control (tourniquet if required)
- Manage for early shock
- Correct packaging: ensure no direct ice contact
- Rapid transport with early notification
- Full documentation including CSM (if applicable), care provided, and tissue handling
Even small amputations (e.g., fingers or toes) carry significant functional impact and require the same systematic approach.
Early, appropriate care directly influences surgical outcomes.
Tip of the Month - April 2026 - Glasgow Coma Scale
"Can you open your eyes for me?"
If a patient opens their eyes when you speak to them, are they automatically a GCS 14?
Not necessarily. Accurate scoring depends on how and why the response occurs
Why This Matters
GCS miscalculations remain common in the field - particularly in Eye Opening and Motor Response scoring.
These errors can impact:
- Clinical decision-making
- Transport priorities
- Accuracy of hospital handover
Key Principles for Accurate Scoring
- Document the best observed response
- Score based on the highest level of function demonstrated
- Identify and communicate trends
- Serial GCS assessment are more valuable than a single score
- Differentiate inability vs. non compliance
- Is the patient unable to respond, or choosing not to?
- Baseline matters
- A patient who is baseline- oriented is a GCS 15, even with pre-existing cognitive impairment
The Golden Rule
A decreasing GCS is an early and critical indicator of patient deterioration.
Factors That Can Interfere with GCS Assessment
- Pre-Existing Conditions
- Language barriers
- Cognitive impairment or developmental delay
- Hearing or speech impairment
- Current Interventions
- Airway management (e.g., intubation, tracheostomy)
- Medications (e.g., sedation, analgesia)
- Acute Illness or Injury
- Facial, orbital, or cranial trauma
- Stroke symptoms (e.g., dysphasia, hemiplegia)
- Spinal cord injury
- Hypoxia
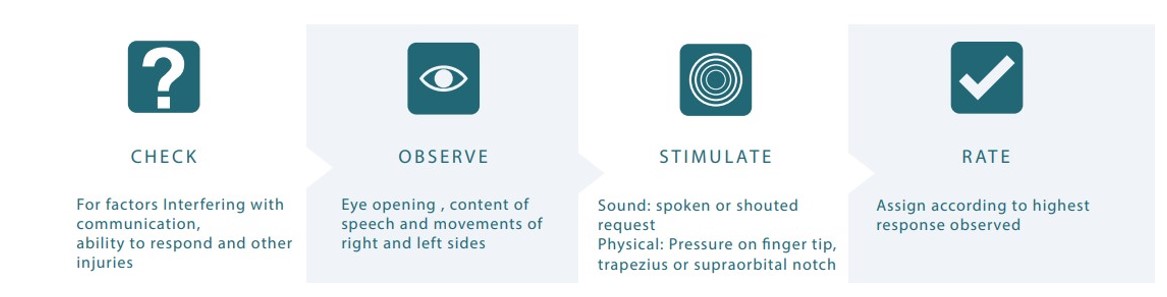
Approach to GCS Assessment 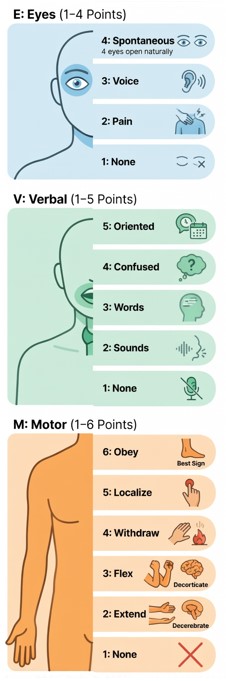
CHECK
Identify factors that may interfere with accuracy
OBSERVE
Look for spontaneous eye opening, speech, and movement
STIMULATE
Progress from verbal → tactile → painful stimuli (only as required)
RATE
Assign GCS based on the best observed response
Additional Resource
For further detail, refer to: Glasgow Coma Scale Foundation
glasgowcomascale.org
March Tip of the Month - Seizures: When Treatment Ends on Scene
Seizures result from abnormal, excessive neuronal activity in the brain and may be provoked (e.g., hypoglycemia, hypoxia, electrolyte imbalance, toxic exposure) or unprovoked (e.g., epilepsy). Seizure presentations vary widely, and not all seizure-like activity represents epileptic disease. Most generalized seizures are self-limiting and resolve within 1 to 2 minutes, followed by a post-ictal period. The role of paramedics is to identify seizure type, treat reversible causes, terminate active seizures when indicated, and determine the appropriate disposition. Under ALS-PCS v5.4, selected patients who have returned to baseline may be considered for treat and discharge, provided strict criteria are met.
By the end of this tip, paramedics will be able to recognize common seizure types and determine which patients meet ALS-PCS criteria for treatment and discharge versus mandatory transport.
You respond to a 27-year-old patient with a known history of epilepsy. Family report a generalized tonic-clonic seizure lasting approximately 90 seconds, consistent with the patient’s usual seizures. On arrival, the seizure has stopped. The patient is initially post-ictal but gradually becomes alert, oriented, and returns to their normal baseline. Vital signs and blood glucose are normal.
Does this person require ongoing care, or are they safe to discharge?
Common seizure types paramedics may encounter include:
- Generalized Seizure
- Sudden LOC, tonic stiffening followed by rhythmic clonic movements
- Often followed by post-ictal phase
- May be epileptic or provoked by metabolic/toxic causes
- Focal (partial) Seizures
- Motor, sensory, or behavioural changes without full loss of consciousness
- Post-ictal confusion may be minimal or absent
- Absence Seizures
- Brief staring spells, typically no post-ictal state
- More common in pediatric population
- Status Epilepticus
- When any seizure lasts more than 5 minutes or when seizures occur very close together and the person does not recover consciousness between them
- Physcogenic Nonepileptic Seizures (Functional Seizures)
- Prolonged or fluctuating episodes
- Eye tightening, crying, talking, or purposeful movement
- Rapid return to baseline
Important note: PNES are real medical events, not intentional or “faked”. Management focuses on patient reassurance, assessment for injury or medical illness, and disposition based on overall presentation.
Treat and discharge is an appropriate, evidence-based outcome for select seizure patients who fully recover and meet ALS-PCS criteria. Recall your IDEAL discharge planning framework:
I - Incldue the patient and family as full partners
- Engage the patient and caregivers early
- Confirm who will assist at home
- Encourage questions
- Avoid provider-only decision making
D - Discuss key areas
Specifically:
- Medications (changes, new prescriptions, stopped meds)
- Warning signs and symptoms
- Follow-up appointments
- Daily living needs
- Test results
E - Educate using teach-back
- Use plain language
- Ask the patient to repeat instructions in their own words
- Clarify misunderstandings immediately
- Provide written instructions (if required)
A - Assess understanding and barriers
- Health literacy
- Transportation
- Financial constraints
- Home supports
- Cognitive limitations
L - Listen to and honor patient preferences
- Cultural considerations
- Goals of care
- Capacity and autonomy
- Feasibility of the plan
When a patient with known epilepsy returns to baseline after a typical seizure, consider how applying ALS-PCS criteria can safely support treat and discharge as the right clinical decision.
February Tip of the Month - Owning the Outcome: Ethics, Failure, and Legal Responsibility
Talking about mistakes and failure isn’t something we do often enough. As humans, we naturally appreciate being recognized for what we do well, but let’s be honest, no one enjoys having their flaws or errors pointed out. The truth is simple: everyone makes mistakes. Yes, everyone.
This topic is not meant to intimidate, assign blame, or act as a scare tactic. Its purpose is to create clarity, encourage honest reflection, and support growth. The framework focuses on professionalism, ethical practice, documentation integrity, patient advocacy, and accountability because learning from mistakes is how we strengthen ourselves, our practice, and the trust placed in us.
Objective:
By the end of this tip, paramedics will have a clearer understanding of ethical and professional standards, gain insight into accountability and documentation practices, strengthen patient advocacy and escalation of care, and reflect on expectations that support positive and meaningful practice change.
Key Content:
Professionalism
Professionalism is reflected in how you act when things don’t go as planned. It includes honesty, respect, humility, and a willingness to acknowledge mistakes. Owning your actions especially during challenging calls demonstrates integrity and reinforces trust within your teams and with the public.
Ethical Practice
Ethical practice requires you to place patient safety and well-being at the center of every decision. When errors or near misses occur, ethics guide you to be transparent, reflective, and committed to improvement rather than avoidance or defensiveness.
Documentation Integrity
Accurate, timely, and truthful documentation is essential. Ambulance Call Reports (ACRs) tell the story of your clinical decision-making and are critical for continuity of care, quality improvement, and legal accountability. Documentation should always reflect what actually occurred and not what you wish had happened.
Patient Advocacy
Advocating for patients means speaking up when something doesn’t feel right, reassessing when conditions change, and escalating care when needed. Advocacy is not about questioning competence, it’s about ensuring patients receive the safest and most appropriate care possible.
Accountability
Accountability is not about punishment, it is about responsibility. Taking ownership of your actions, learning from mistakes, and making changes when needed. This strengthens both individual practice and the profession as a whole. Accountability helps maintain public trust and supports a culture of safety and learning.
Scenario:
A 78-year-old patient with a head injury and on blood thinners refuses transport after a fall. Pressured by family, short on time, and facing a busy system, the crew accepts a quick refusal with minimal risk explanation and limited documentation. Hours later, the patient deteriorates and dies from an intracranial bleed. The crew is later subpoenaed.
Patient refusals are not just about assessing orientation, quantifying vitals and obtaining signatures. High-risk patients require a clear capacity assessment, thorough explanation of risks in plain language, freedom from outside influence, and strong documentation. Rushed decisions and “checkbox refusals” can turn ethical shortcuts into legal consequences.
Remember, if you wouldn’t feel comfortable reading your ACR out loud in court, it’s not finished.
In paramedicine, ethical care isn’t just about getting it right, it’s about what you do when things go wrong. Failure can sting, especially in a profession shaped by legal accountability and public trust. But reflective practice asks you to look squarely at your decisions: the pressures you faced, the information you had, the biases you carried, and the systems around you. Owning mistakes doesn’t weaken professionalism, it strengthens it by turning accountability into learning, protecting patients, and safeguarding your future practice.
Challenge: Think of a recent call that didn’t sit right. What would you do differently next time, and what support or system change would help you do it?
Previous Articles
-
May 2026 - Tip of the Month - Amputations
-
Tip of the Month - April 2026 - Glasgow Coma Scale
-
March Tip of the Month - Seizures: When Treatment Ends on Scene
-
February Tip of the Month - Owning the Outcome: Ethics, Failure, and Legal Responsibility
-
January Tip of the Month - Mean Arterial Pressure "MAP" - The Rule of 65
-
**AMENDED** Winter Emergencies: Recognition and Care for Hypothermia and Frostbite
-
November Tip of the Month - Not "Just" the Flu: Recognizing High-Risk Respiratory Illness
-
October Tip of the Month - Diabetic Emergencies
-
September Tip of the Month - Sepsis
-
August Tip of the Month - Mass Casualty Incidents
